Dementia is one of the most misunderstood health problems because it often starts quietly. A forgotten appointment, a misplaced key, or a repeated question may look harmless at first, but the deeper concern arises when these changes begin to disturb daily life, judgment, communication, safety, or personality. We should treat dementia as more than “just memory loss” because it is a group of symptoms caused by different diseases and brain changes, and some dementia like symptoms can improve when the cause is found and treated. Mayo Clinic
The most important truth is simple. Dementia is not a normal part of aging, even though age remains the strongest known risk factor. We may forget a name and remember it later as we grow older, but dementia can make a person lose track of familiar places, struggle with basic decisions, repeat questions without awareness, or behave in ways that feel unlike them.
What Dementia Really Means

Dementia is an umbrella term for a decline in thinking, memory, reasoning, language, behavior, or social ability that becomes strong enough to interfere with everyday life. It is not one single disease. Alzheimer’s disease is the most common cause, but vascular dementia, Lewy body dementia, frontotemporal dementia, Parkinson’s disease dementia, traumatic brain injury, and mixed dementia can also create dementia symptoms.
We should think of dementia as a signal that the brain’s communication system is being damaged. Nerve cells and their connections may be injured, lost, deprived of blood supply, affected by abnormal protein buildup, or disturbed by another medical condition. The symptoms depend on which brain areas are affected, which is why one person may first show memory problems, another may show personality changes, and another may struggle with movement, focus, or language.
Dementia Symptoms That Often Appear First
Early dementia symptoms can be subtle because families often explain them away as stress, tiredness, grief, aging, or distraction. The warning sign is not a single forgotten detail. The warning sign is a pattern that grows, repeats, and begins to affect independence, relationships, work, money, driving, cooking, medication use, or safety.
Common early signs include forgetting recent events, losing items often, getting confused in familiar places, losing track of dates or time, struggling to solve problems, having trouble following conversations, finding it hard to complete familiar tasks, and misjudging distance or space. Mood and behavior can also shift early, with anxiety, sadness, anger, withdrawal, personality changes, or reduced interest in other people’s emotions. World Health Organization
Cognitive Warning Signs of Dementia
Cognitive symptoms affect how a person thinks, learns, remembers, plans, and responds to everyday problems. These symptoms often create the first practical trouble families notice. A person may forget appointments, struggle to follow a recipe, lose the thread of a conversation, repeat questions, make unusual financial choices, or become overwhelmed by multi-step tasks.
Problems with language can be especially frustrating. Someone may pause often to find simple words, use the wrong word, call objects by vague names, or stop joining conversations because speaking feels harder. Visual and spatial changes may also appear, including trouble judging distance, reading maps, parking, using stairs, or driving safely.
Mood and Personality Changes in Dementia

Dementia can change more than memory. It can affect emotional control, motivation, judgment, social behavior, and personality. A calm person may become suspicious. A careful person may become impulsive. A warm person may seem withdrawn, flat, irritable, anxious, or unusually blunt. These changes can be painful for families because they feel personal, yet they may come from disease activity in the brain.
Depression, anxiety, agitation, paranoia, hallucinations, inappropriate behavior, and personality changes can occur in dementia. Some people see things that are not there, especially in Lewy body dementia. Others act out dreams during sleep, move slowly, develop tremors, or have stiffness. These symptoms deserve medical attention because they can affect safety, sleep, caregiver stress, and quality of life.
Dementia Symptoms Versus Normal Aging
Normal aging may slow recall, but it usually does not erase independence. A person may forget a word and remember it later. They may need more time to learn a new phone, app, or appliance. They may misplace glasses and retrace their steps. Dementia is different because the problem keeps returning and begins to shrink daily functioning.
A useful way to separate normal aging from possible dementia is to ask what has changed. Can the person still manage money, meals, medication, appointments, hygiene, transportation, and social life at their usual level? Are mistakes becoming riskier or more frequent? Are loved ones noticing changes that the person does not recognize? Memory loss that is noticed mainly by others is one of the common dementia warning signs.
These categories matter because dementia is not treated or managed in one single way. Different patterns can point toward different causes, and some symptoms may require a different safety plan, medication review, home routine, or specialist evaluation.
Conditions That Can Look Like Dementia But May Be Treatable
One of the strongest reasons to seek medical care early is that some dementia like symptoms come from treatable problems. Thyroid disease, low blood sugar, abnormal sodium or calcium levels, low vitamin B12, medication side effects, infections, immune disorders, dehydration, subdural bleeding after a fall, brain tumors, and normal pressure hydrocephalus can create symptoms that resemble dementia.
We should never assume that confusion automatically means permanent decline. A person who suddenly becomes confused, sleepy, disoriented, paranoid, or unable to function needs prompt medical evaluation. In older adults, sudden confusion may come from infection, medication effects, dehydration, injury, metabolic problems, or other urgent health changes. Finding the cause can protect the brain and may prevent avoidable decline.
What Causes Dementia in the Brain
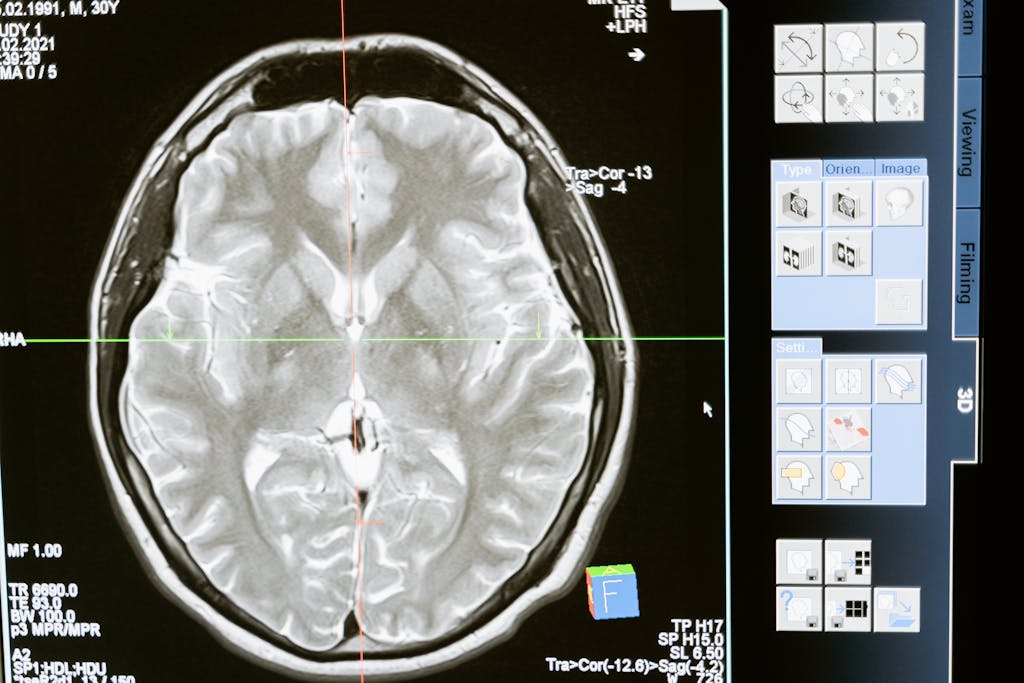
Dementia develops when disease or injury damages brain cells and the connections between them. In Alzheimer’s disease, abnormal protein deposits are strongly associated with brain cell damage. In vascular dementia, blood vessel problems can reduce the brain’s oxygen and nutrient supply. In frontotemporal dementia, damage affects areas tied to behavior, personality, and language. In Lewy body dementia, protein deposits are linked with attention changes, movement symptoms, sleep disturbance, and hallucinations.
This is why dementia can look so different from one person to another. The brain does not handle memory, judgment, movement, mood, vision, and language in one single location. Damage in one network may first disturb speech, while another network may first disturb planning, emotional control, or balance.
Major Risk Factors We Cannot Change.
Age is the biggest risk factor, especially after midlife and later older age, but dementia is still not a normal or guaranteed part of aging. Family history can raise risk, though many people with a family history never develop dementia, and many people without a family history still do. Some genes influence risk, and rare deterministic genes can directly cause younger-onset dementia in a small share of cases. Alzheimer’s Disease International
Down syndrome is also linked with a higher risk of earlier Alzheimer’s disease in adulthood. Severe or repeated traumatic brain injury can raise dementia risk as well, especially when head injuries are multiple or serious. These factors cannot always be removed, but knowing them can help families take symptoms seriously and seek evaluation earlier.
Dementia Risk Factors We Can Work On
Many dementia risks are connected to heart health, lifestyle, hearing, mood, and the environment. Known risk factors include physical inactivity, uncontrolled diabetes, high blood pressure, hearing loss, tobacco use, and alcohol use. Other risk factors include obesity, depression, social isolation, cognitive inactivity, high cholesterol, air pollution, head injury, untreated vision loss, and low educational exposure across the life course.
This does not mean dementia is anyone’s fault. Risk is shaped by biology, income, neighborhood safety, food access, health care access, education, pollution, work conditions, and family history. Still, the hopeful part is real. Research summaries suggest that a large share of dementia cases may be preventable or delayed when modifiable risks are addressed across individuals and society.
How Heart Health Protects Brain Health
The brain depends on steady blood flow. High blood pressure, diabetes, smoking, obesity, high cholesterol, stroke, and blood vessel disease can damage the flow over time. This is why dementia prevention often overlaps with heart disease prevention. What protects the arteries often protects the brain.
Managing blood pressure, blood sugar, cholesterol, weight, smoking, physical activity, and alcohol use can help reduce risk. Physical activity supports the heart, circulation, balance, mood, sleep, and independence. Adults are commonly encouraged to aim for 150 minutes of physical activity each week, with adjustments for health status and medical advice.
Hearing, Vision, and Social Connection Matter More Than Many Families Realize
Hearing loss is now treated as a major dementia risk factor. When hearing becomes difficult, the brain may work harder to decode sound, conversations become tiring, and social withdrawal can follow. Treating hearing loss with professional support may reduce dementia risk and improve communication, safety, and quality of life. (CDC)
Vision loss also deserves attention because untreated vision problems can reduce independence, movement, reading, confidence, and social engagement. We should also take loneliness seriously. Social connection, meaningful activity, conversation, learning, hobbies, and community involvement may support cognitive reserve and emotional health. (Alzheimer’s Disease International)
How Dementia Is Diagnosed
No single test can diagnose all dementias. A good evaluation usually begins with medical history, symptom history, medication review, physical exam, and input from someone who knows the person well. Cognitive and neuropsychological tests may measure memory, attention, reasoning, language, orientation, and judgment. Neurological evaluation may check balance, movement, reflexes, senses, and coordination. (Mayo Clinic)
Brain scans such as CT or MRI can look for stroke, bleeding, tumors, or fluid buildup. PET scans may show brain activity patterns or Alzheimer’s related amyloid or tau deposits. Blood tests may check for thyroid problems, low vitamin B12, infection markers, metabolic issues, or other conditions affecting brain function. A psychiatric exam may help identify depression or another mental health condition contributing to symptoms. (Mayo Clinic)
Why Early Dementia Diagnosis Can Change the Road Ahead
Early diagnosis gives families time. It can uncover treatable causes, improve medication safety, reduce driving or cooking risks, support legal and financial planning, and help the person express care preferences before symptoms become more advanced. It can also connect families with occupational therapy, caregiver training, support groups, home safety planning, and symptom management.
For some people with early Alzheimer’s disease or mild cognitive impairment due to Alzheimer’s, newer treatments may be discussed with a specialist. These medicines are not for everyone and can carry serious risks, including brain swelling or bleeding, so evaluation, monitoring, and careful selection matter. (Mayo Clinic)
Dementia Treatment and Symptom Management
Most types of dementia cannot currently be cured, but symptoms can often be managed. Some medicines may temporarily improve or stabilize symptoms in certain people, including cholinesterase inhibitors and memantine. Other medicines may be used for depression, sleep problems, hallucinations, agitation, or movement symptoms when needed. Medication decisions should be individualized because side effects and drug interactions can be serious in older adults. (Mayo Clinic)
Therapies and routine changes can be just as important as prescriptions. Occupational therapy can help make the home safer and reduce falls. Lower clutter and noise can improve focus. Breaking tasks into smaller steps can reduce frustration. A predictable daily routine can help the person feel more secure, especially as memory and orientation become harder. (Mayo Clinic)
Home Safety Changes That Protect People With Dementia
Dementia can turn ordinary household tasks into safety risks. Cooking, driving, walking outside alone, using tools, taking medications, bathing, and managing money may become difficult. Families should look for warning signs such as burned pans, expired food, missed medication, unpaid bills, wandering, falls, dents on the car, or confusion at night.
Helpful changes include simplifying the home, labeling important spaces, removing trip hazards, securing dangerous objects, using medication organizers, improving lighting, setting routines, and creating calm evening habits. Monitoring systems may help when wandering becomes a concern. The goal is not to take dignity away. The goal is to reduce danger while preserving as much independence as possible. (Mayo Clinic)
Communication Strategies That Reduce Conflict
Dementia changes how a person processes information, so communication must become slower, warmer, and simpler. We should use short sentences, one idea at a time, gentle eye contact, familiar words, and visual cues. Arguing over incorrect memories usually increases distress. Redirecting with respect often works better than correcting every detail.
A person with dementia may ask the same question because the answer does not stay. They may refuse help because they feel embarrassed, afraid, or confused. They may become angry because the world suddenly feels unpredictable. We should respond to the emotion first, then guide the task with patience.
Dementia Complications Families Should Prepare For
As dementia progresses, the person may need help with bathing, dressing, toileting, grooming, eating, medication, and mobility. Poor nutrition can develop when appetite drops or chewing and swallowing become difficult. Swallowing problems can raise the risk of choking or aspiration pneumonia. Safety risks may grow around driving, cooking, falls, wandering, and living alone. (Mayo Clinic)
Planning early makes these changes less chaotic. Families should discuss advance care preferences, legal documents, financial access, medical decision makers, home care options, transportation, and long term support. These conversations are easier before a crisis forces rushed decisions.
Dementia Prevention Steps We Should Start Earlier
There is no guaranteed way to prevent dementia, but risk reduction is still powerful. We should protect the brain by staying physically active, avoiding smoking, limiting harmful alcohol use, managing weight, eating a healthy diet, treating high blood pressure, controlling blood sugar, managing cholesterol, addressing depression, protecting hearing and vision, staying socially connected, reducing head injury risks, and keeping the mind active. (World Health Organization)
A Mediterranean style eating pattern is often linked with better cardiovascular and cognitive health. This pattern emphasizes vegetables, fruits, whole grains, nuts, olive oil, fish, and smaller amounts of meat and dairy. The brain benefits most from a full lifestyle approach rather than one miracle food, one supplement, or one expensive habit. (Mayo Clinic)
When We Should See a Doctor
A medical visit is important when memory problems, confusion, personality changes, word finding trouble, poor judgment, hallucinations, movement changes, or daily task problems begin affecting life. It is also important when loved ones notice changes the person does not see. Some causes can be treated, and even progressive dementia benefits from earlier planning and support. (Mayo Clinic)
Urgent care is needed when confusion appears suddenly, worsens quickly, follows a fall or head injury, comes with fever, severe headache, weakness, facial drooping, chest pain, fainting, seizure, severe dehydration, or sudden behavior change. Sudden confusion is not typical dementia progression until other urgent causes have been considered.
Key Takeaway
Dementia is not ordinary aging, and it is not only forgetfulness. It is a serious change in memory, thinking, behavior, communication, movement, or daily function that deserves careful medical attention. Some causes can be treated, some symptoms can be managed, and many risks can be reduced through earlier action.
We should watch patterns, not isolated mistakes. When a loved one changes in ways that affect safety, independence, personality, judgment, or communication, the right response is not fear or denial. The right response is evaluation, planning, support, and steady care that protects both the person and the family around them.






